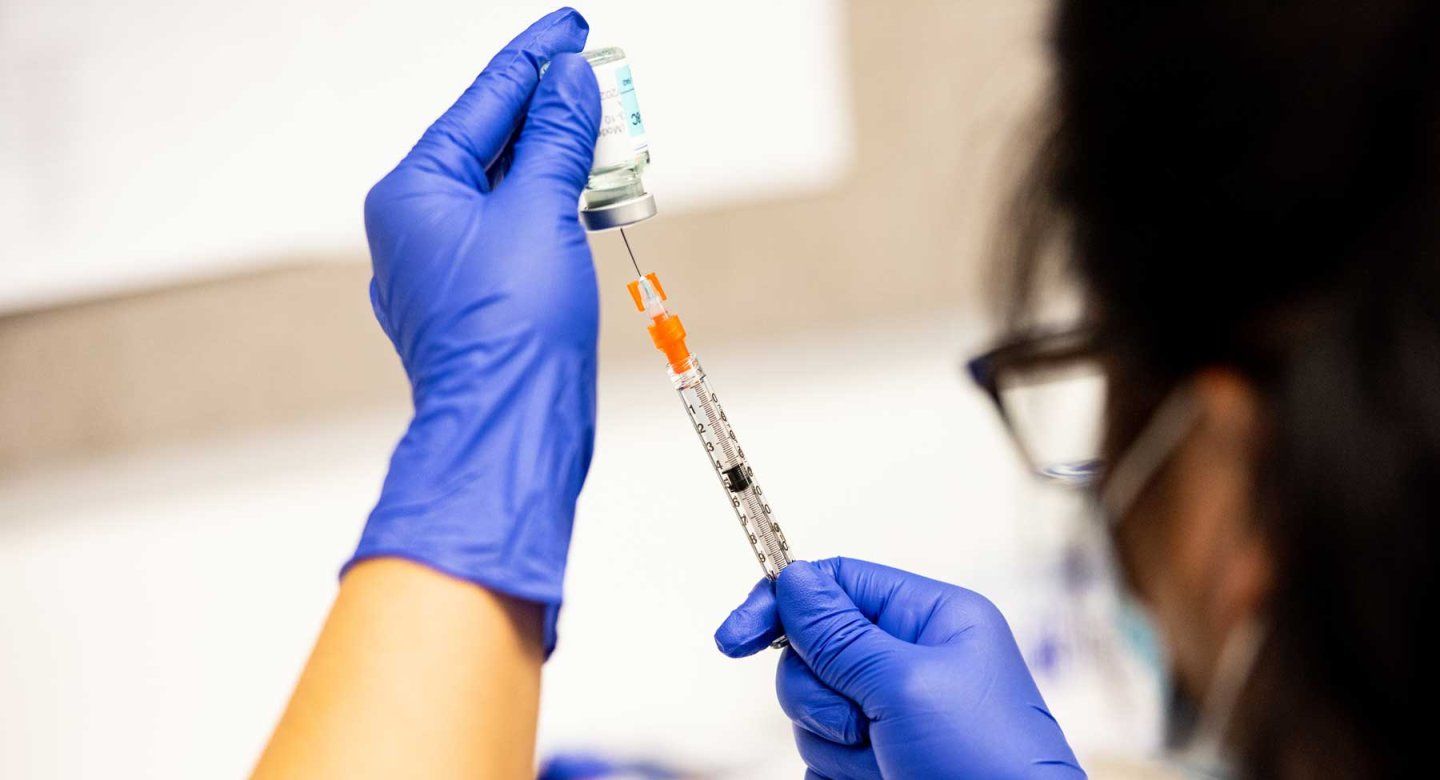
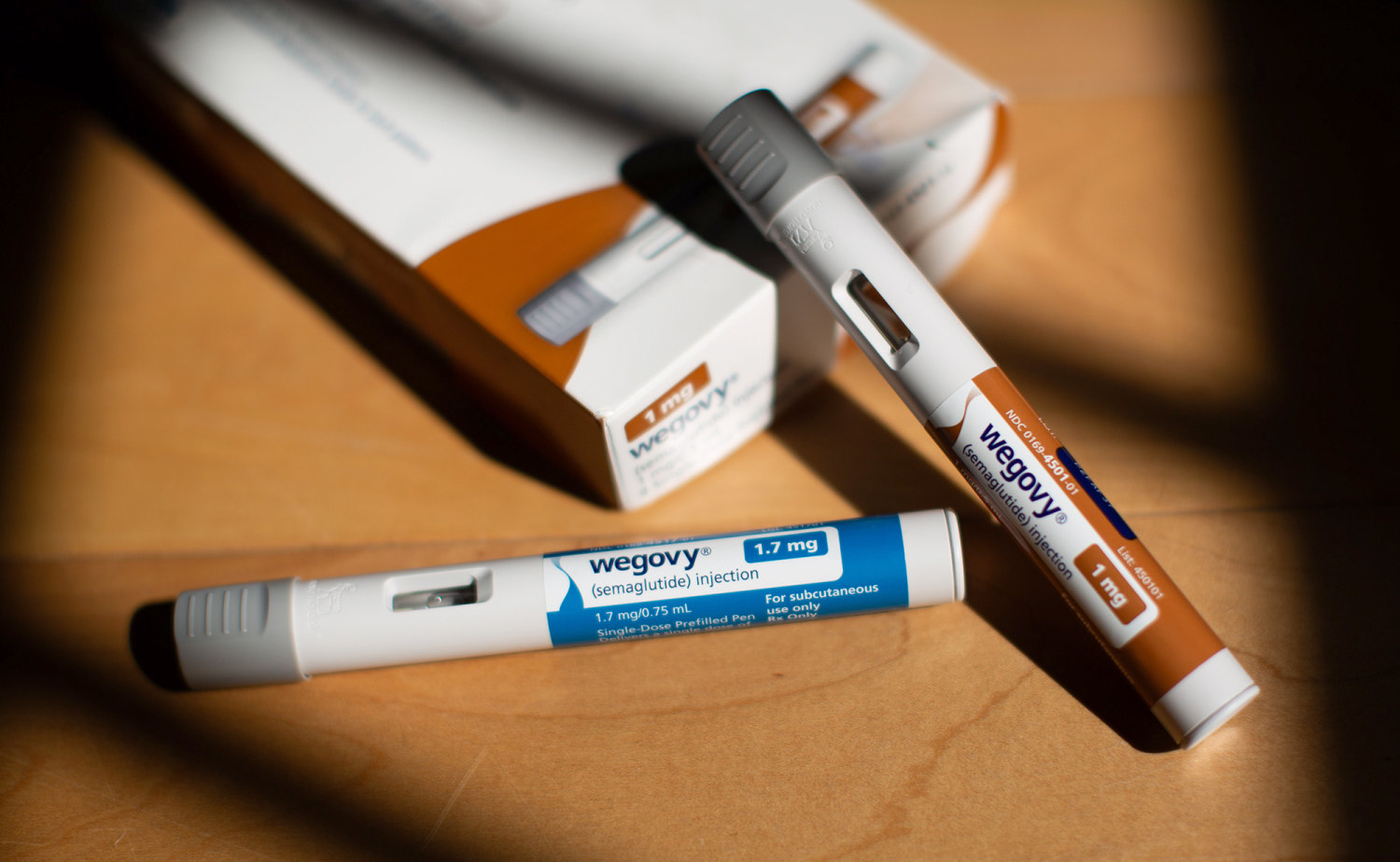
As summer unfolds, COVID-19 infections are once again on the rise in various parts of the United States. While not reaching the alarming levels of previous years, the recent uptick in cases is noticeable enough to revive conversations around preventive measures—especially the potential need for updated vaccines.
Esta reaparición estacional ha sido detectada a través de un incremento en los niveles de partículas virales en los sistemas de vigilancia de aguas residuales, un indicador anticipado confiable de la propagación comunitaria. Las visitas a los departamentos de emergencia y las hospitalizaciones también han mostrado un aumento leve pero constante. Aunque la situación está lejos de ser crítica, el cambio es lo suficientemente significativo como para merecer atención, especialmente para aquellos en categorías de alto riesgo, como los ancianos y los inmunocomprometidos.
Grasping the summer wave
Unlike the early stages of the pandemic, the current increase in COVID-19 activity is not accompanied by widespread panic or drastic public health mandates. This is largely due to a population that has developed a certain level of immunity through vaccinations, past infections, or both. However, the virus continues to evolve, and new variants can evade some of the immune protection previously acquired.
The prevalent forms currently are subvariants of the Omicron family, recognized for their increased transmissibility yet less propensity to lead to severe illness in people who have some kind of immunity. Nonetheless, the virus continues to be a hazard, especially for those at risk or with existing health issues. Despite this, individuals in good health can also endure prolonged symptoms, referred to as long COVID, after getting infected.
Vaccine timing: to boost or not to boost?
One of the primary questions emerging from this latest rise in cases is whether it’s the right time for a booster shot. Health authorities are preparing for a fall vaccination campaign that will likely offer updated COVID-19 vaccines, targeting newer variants more effectively. However, for those currently at heightened risk of severe illness, waiting might not be the best option.
Experts are divided. On one hand, individuals who are elderly, chronically ill, or immunocompromised may benefit from an additional booster now, particularly if it’s been several months since their last dose. This could help bridge the gap until the next round of updated vaccines becomes available. On the other hand, those at lower risk may choose to wait until the fall to receive a booster that’s tailored to the currently circulating variants.
The decision largely depends on individual risk factors and timing. For many, it’s a matter of balancing protection now against potentially better protection later. For example, someone planning to travel, attend large gatherings, or spend time indoors in close proximity to others might opt for a booster to reduce the risk of infection and transmission in the immediate term.
Public response and prevention measures
Although the number of cases is rising, the general populace seems to be less worried compared to earlier surges. The use of masks is inconsistent, and numerous individuals have stopped maintaining social distance or steering clear of packed indoor areas. This change in conduct indicates a widespread feeling of weariness with pandemic measures and a longing to resume normal life.
Still, some precautionary steps continue to be useful. Proper ventilation, wearing masks in packed places, maintaining hand cleanliness, and staying home when showing symptoms can still help limit the virus’s spread. The present increase acts as a reminder that the pandemic, though less intrusive than it once was, isn’t entirely over.
The evolving nature of COVID-19
COVID-19 continues to be unpredictable. While vaccines have significantly reduced the likelihood of severe disease and death, the virus’s ability to mutate means that no single strategy offers complete protection indefinitely. The rise of new subvariants and the potential for future surges, especially during the colder months, highlight the need for ongoing vigilance and adaptability in public health strategies.
For many, COVID-19 has transitioned from a once-dreaded virus to a recurring seasonal illness—more like the flu than the threat it once posed. But unlike the flu, COVID-19 continues to present unique challenges, particularly because of the lingering effects experienced by some patients.
What you can anticipate
With the fall season approaching, public health officials are closely monitoring the situation. Updated vaccines are expected to be rolled out later in the year, likely in a formulation better matched to the latest variants. These will probably be offered alongside the annual flu vaccine, and possibly the RSV vaccine for certain age groups, as part of a broader strategy to tackle respiratory illnesses.
In the interim, individuals at higher risk are advised to speak with their medical professionals about the possibility of an extra booster before autumn. For everyone else, keeping updated and following simple preventive measures continues to be the wisest approach as circumstances change.
The recent summer spike in COVID-19 serves as a subtle but important reminder: while the virus no longer dominates daily life, it still requires attention, especially when community transmission begins to climb. As science continues to adapt to a changing virus, individuals are once again faced with the task of making informed choices to protect themselves and those around them.